Eczema, a term that encompasses a range of persistent skin conditions, manifests in several distinct forms, including atopic dermatitis, contact dermatitis, dyshidrotic eczema, nummular eczema, seborrheic dermatitis, and stasis dermatitis.
In this article, we explore each of these types of eczema in detail, uncovering their specific symptoms, causes, and treatment strategies to provide a clearer understanding of this complex and often challenging skin condition.
Common Types of Eczema
Eczema, a group of conditions that cause skin inflammation and irritation of the skin, includes several common types, each with different characteristics and causes of eczema.
Atopic Dermatitis
Atopic dermatitis, commonly known as eczema, is a chronic inflammatory skin condition typically appearing in early childhood. It causes red, scaly, and itchy patches of skin, sometimes accompanied by tiny fluid-filled blisters that may weep if infected, often by Staphylococcus aureus. This type of eczema is not contagious.
Symptoms of atopic dermatitis can vary in intensity, with flare-ups and periods of remission. If symptoms worsen, disrupt sleep, or show signs of infection, it’s advisable to consult a doctor promptly.¹
Contact Dermatitis
Contact dermatitis is inflammation of the skin triggered by contact with a specific substance. There are two main types of contact dermatitis:
- Allergic contact dermatitis: Caused by an allergen, each exposure to the allergen leads to skin inflammation.
- Irritant contact dermatitis: Occurs when the skin becomes inflamed after prolonged exposure to an irritant substance.
Symptoms of contact dermatitis include cracked skin, redness, blisters, thickened skin, dryness, and itching.²
Dyshidrotic Eczema
Dyshidrotic eczema (DE), also referred to as acute palmoplantar eczema, is a common skin condition that often affects adults, causing dermatitis on the hands and feet. This type of eczema is characterised by recurring outbreaks of small, fluid-filled blisters that can appear suddenly and are intensely itchy. One of its hallmark features is the resemblance to “tapioca pudding”. DE tends to occur more frequently in younger adults and affects both men and women equally.³
Nummular Eczema
Nummular dermatitis, also known as discoid eczema or nummular eczema, is a type of itchy skin condition characterised by multiple round or coin-shaped lesions. These lesions can vary in size and are typically found on the arms and legs, though they may also appear on the trunk, albeit less commonly.⁴
Seborrheic Dermatitis
Seborrheic dermatitis, also spelled seborrhoeic dermatitis, is a type of skin inflammation that typically affects areas of the body where sebum, an oily substance, is produced in abundance. Common areas include the scalp, face, and torso.
This condition, also known as seborrheic eczema, often manifests as patches of skin that appear oily, flaky, or scaly. On the scalp, particularly in infants, it can cause crusting yellow sores, a condition referred to as cradle cap. The affected skin may also be red, itchy, or sensitive.⁵
Stasis Dermatitis
Stasis dermatitis is a long-lasting skin condition that mainly affects older people’s legs who have a problem with their veins called chronic venous insufficiency. This happens when veins struggle to send blood from the legs back to the heart. The condition is due to increased pressure in the veins, leading to symptoms like skin discolouration, itching, dryness, and scaling. These can look a lot like cellulitis (a bacterial skin infection causing redness, swelling, and pain) or allergic contact dermatitis (an itchy rash from touching something irritating).⁶
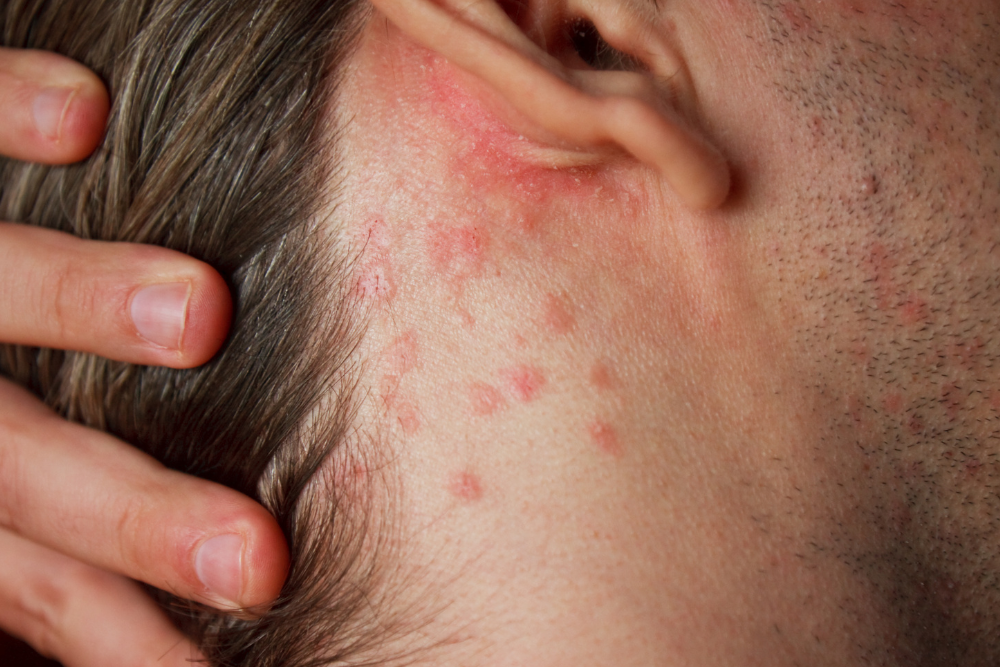
Diagnosis
Diagnosis of eczema is primarily based on a physical examination and a review of personal and family medical history. There are no specific tests for eczema, but certain procedures can help differentiate it from other skin conditions:
Patch Testing
Commonly used to diagnose contact dermatitis by applying small amounts of various substances to the skin and observing reactions.
Skin Swab
Skin swabs may be used to rule out infection, especially if the eczema is severe or doesn’t respond to treatment.
Blood Tests
Blood tests can be helpful in identifying underlying conditions, such as allergies, that may contribute to eczema symptoms.
Skin Biopsy
Rarely needed but can be used to exclude other conditions with similar symptoms. Learn the differences between psoriasis and eczema.
A dermatologist or healthcare provider will consider the appearance of the skin and the history of symptoms. Since eczema can often be confused with other skin disorders, like psoriasis, a careful examination is essential for an accurate diagnosis.

Eczema Treatments
Eczema treatment aims to heal the affected skin and prevent flares. Since eczema varies from person to person, treatments must often be tailored to individual needs.
Treatment options for eczema include moisturisers (emollients), anti-inflammatory ointments like corticosteroids or non-steroidal options, coal tar to relieve itching (though it can stain and irritate), dietary changes (with professional guidance), ultraviolet radiation therapy (phototherapy), and in severe cases, oral medications. Emollients help keep the skin hydrated, best applied after bathing or in dry environments. Corticosteroids are effective but should be used in the lowest effective strength to avoid side effects like skin thinning. Oral corticosteroids are a last resort due to serious potential side effects. Newer treatments like biologics are also emerging for severe cases. Treating eczema early and effectively may reduce the risk of developing allergies like food allergies, asthma, and hay fever later in life.¹
It’s essential to work with a healthcare provider to determine the most effective treatment plan, as what works for one person may not be as effective for another. Regular follow-ups and adjustments to the treatment plan are often necessary to manage eczema effectively over time.

Coping with Eczema
Managing eczema involves making adjustments to daily habits that can aggravate symptoms. Factors like hot weather, frequent showering, certain soaps, and environmental conditions like central heating can worsen eczema.¹ Here are practical tips to help manage eczema and reduce flare-ups:
Good Hygiene
- Take lukewarm baths or showers instead of hot ones.
- Avoid ordinary soap; use soap-free products or sorbolene cream for sensitive areas.
- Use bath oils to moisturise skin while bathing.
- Pat skin dry gently with a towel instead of rubbing.
Reducing Skin Irritation
- Wear breathable layers of clothing and avoid overheating.
- Steer clear of perfumed or medicated bath products.
- Opt for soft fabrics like 100% cotton; avoid scratchy materials like wool or polyester.
- Wear protective gloves when using chemicals or detergents.
Beauty Products
- Minimise the use of hypoallergenic cosmetics and avoid perfumes or fragranced lotions.
- Test new cosmetics on a small area of skin before regular use.
Allergies
- Consider allergy testing if resistant eczema persists, to identify triggers like dust mites or pollen.
Temperature Changes
- Gradually adjust to temperature changes to avoid skin irritation.
- Limit physical activity in extreme temperatures to prevent sweating, which can trigger itching.
Diet
- While diet typically doesn’t cause eczema, some individuals may find certain foods worsen symptoms. Seek advice from a doctor or dietitian for allergy testing and dietary adjustments.
General Tips
- Keep fingernails short to prevent skin damage from scratching.
- Consider a water-softening device if your water is hard or alkaline.
- Swim in seawater when possible, as it may alleviate symptoms.
- Use sun exposure cautiously; while it can help, excessive exposure can harm skin.
Always consult with a healthcare professional for personalised advice on managing eczema effectively. This information is meant for general guidance and should not substitute professional medical advice or treatment.
Seeking Professional Help
Seeking help from a healthcare professional is vital for managing eczema, particularly when self-care isn’t enough. If eczema symptoms persist, get worse, or affect your daily life and mental health, it’s important to see a doctor.
Dermatologists, experts in skin conditions, can give a detailed diagnosis and create a treatment plan suited to you. They’ll also guide you on lifestyle changes and skincare to help control symptoms. If eczema leads to sleep problems, a lot of discomfort, or mental stress, you might need to see specialists like allergists, immunologists, or mental health experts. These professionals can deal with any allergies, immune system issues, or mental health factors linked to your eczema. Getting help early and regularly can control eczema better and prevent more serious problems, improving your quality of life.
Manage eczema flare-ups. Start a hub.health consultation now!
References
- Better Health Channel. Eczema (atopic dermatitis) [Internet]. Melbourne: Victorian Government; [updated 2022 Jan 11; cited 2024 Jun 13]. Available from: https://www.betterhealth.vic.gov.au/health/conditionsandtreatments/eczema-atopic-dermatitis
- Healthdirect Australia. Contact dermatitis – treatments, symptoms and prevention [Internet]. Sydney: Australian Government Department of Health; [updated 2024 Jun 11; cited 2024 Jun 13]. Available from: https://www.healthdirect.gov.au/contact-dermatitis
- National Institutes of Health. Dyshidrotic Eczema: A Common Cause of Palmar Dermatitis [Internet]. Bethesda (MD): PubMed Central; [cited 2024 Jun 13]. Available from: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC
- National Center for Biotechnology Information. Nummular Dermatitis – StatPearls [Internet]. Bethesda (MD): NCBI Bookshelf; [updated 2023 Dec 13; cited 2024 Jun 13]. Available from: https://www.ncbi.nlm.nih.gov/books/NBK
- Healthdirect Australia. Seborrhoeic dermatitis – treatment and causes [Internet]. Sydney: Australian Government Department of Health; [updated 2024 May 15; cited 2024 Jun 13]. Available from: https://www.healthdirect.gov.au/seborrhoeic-dermatitis
- National Institutes of Health. Stasis Dermatitis: An Overview of Its Clinical Presentation, Pathogenesis, and Management [Internet]. Bethesda (MD): PubMed Central; [cited 2024 Jun 13]. Available from: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC




