Confused about ‘dermatitis vs eczema’? Turns out you’re not the only one. Broadly, dermatitis is any skin inflammation, while eczema is particularly characterised by itchy, inflamed skin. This guide cuts through the confusion, showcasing what sets them apart and how they overlap, to help you find relief for your skin.
Key Takeaways
Dermatitis is an inflammation of the skin, which includes eczema, but eczema specifically refers to a group of conditions with itchy and inflamed skin, such as atopic dermatitis.
Atopic dermatitis is a chronic, non-contagious skin condition often related to genetic factors and can be triggered by environmental allergens. Treatment may involve moisturising, corticosteroids, and for severe cases, biologics.
Contact dermatitis is a form of skin inflammation caused by allergens or irritants, leading to symptoms like an itchy rash with a distinct border where contact occurred. Treatment includes topical steroids, oral medications, and avoiding triggers.
Dermatitis and Eczema: Defining the Terms
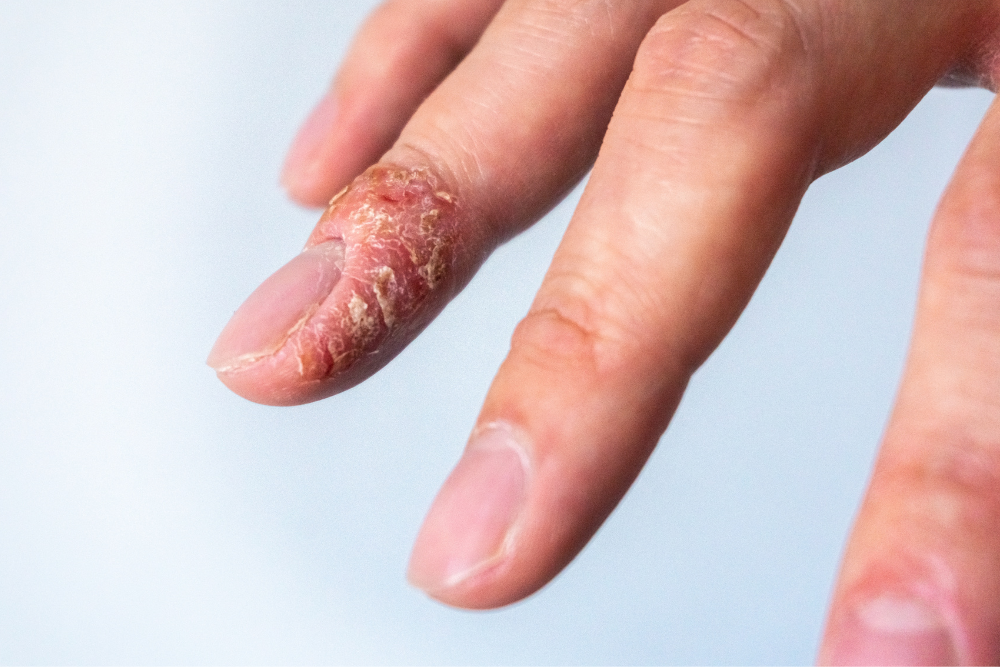
“Dermatitis” is a broad term that refers to inflammation of the skin, encompassing conditions such as eczema. Eczema refers to a group of conditions that are characterised by itchy, dry, and inflamed skin. This condition is commonly found in both children and adults. So, while all eczema is dermatitis, not all dermatitis is eczema.
Eczema and dermatitis are sometimes used interchangeably, but they actually refer to different skin conditions. Eczema is a specific type of dermatitis that causes inflamed, itchy skin. However, some specific conditions are more accurately described by one term over the other. For instance, symptoms of dermatitis can include redness, itching, blistering, and peeling, while eczema, especially atopic dermatitis, the most common type, is noted for itchy, flaky or scaly rashes, and particularly dry skin.
Atopic Dermatitis: A Closer Look
Let’s take a closer look at atopic dermatitis. Often triggered by gene mutations, this type of eczema is noted for its characteristic skin irritation and skin inflammation.
You’ll find it’s not contagious but can be quite bothersome due to the itchy skin rash it produces.
Causes
Atopic dermatitis, also known as atopic eczema, can be exacerbated by a gene variation that leads to a compromised skin barrier function, causing increased skin sensitivity. If your family has a history of severe atopic dermatitis or:
Eczema
Asthma
Allergies
There’s a higher genetic propensity for developing Atopic Dermatitis.
Environmental allergens such as:
House dust mites
Animal dander
Pollen
Moulds
are known to trigger atopic dermatitis flare-ups. Additionally, an overgrowth of Staphylococcus aureus on the skin can disrupt the barrier function, resulting in immune system response and inflamed skin characteristic of atopic dermatitis.
Certain food allergies, including reactions to peanuts, dairy, and eggs, may precipitate or intensify eczema symptoms. Learn about the foods to avoid with eczema.
Symptoms
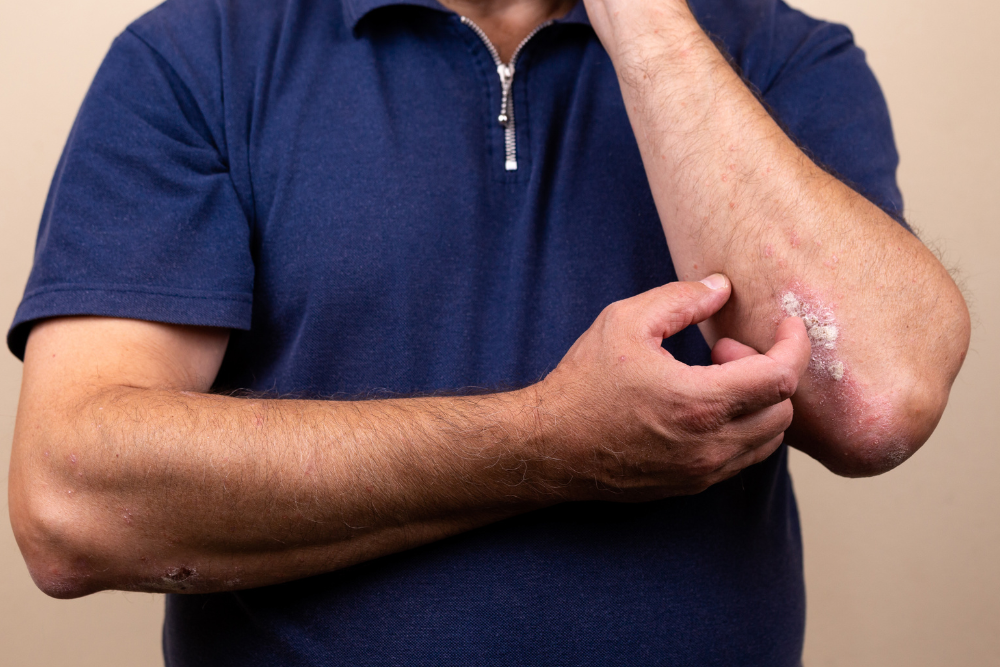
The symptoms of atopic dermatitis can be quite diverse, characterised by general symptoms such as itchy, red, inflamed, and often dry skin. The presentation of these symptoms varies with age. Infants may display a red rash on the face and scalp, children usually have a thickened rash in specific areas like elbows and knees, and teenagers and adults often have a scaly rash on hands, neck, and ankles.
Moreover, hormonal changes and having dry skin can exacerbate the symptoms of atopic dermatitis, making the skin itchier and more sore. It’s not just a mere skin condition; it’s a chronic skin condition that requires careful handling and treatment.
Treatments
When it comes to managing atopic dermatitis, self-care measures are paramount. Regular bathing, moisturising with hypoallergenic products, and self-monitoring for infections can relieve itching and help prevent new outbreaks. For flare-ups, corticosteroid creams and ointments, prescribed either topically or orally, are commonly used.
For moderate to severe cases unresponsive to other treatments, new systemic options like biologic therapy is available.
Contact Dermatitis: An Allergic Reaction
While atopic dermatitis is a prevalent type of eczema, let’s not forget about contact dermatitis. This type of dermatitis is often preventable through the avoidance of irritants and is characterised by an allergic reaction to substances such as cosmetics, fragrances, and plants.
The lesions from contact dermatitis are hallmarked by a clear visible border in the area which was exposed to the irritant, accompanied by an itchy rash.
Causes
Contact dermatitis is triggered by a variety of common allergens and irritants. Allergens that commonly cause allergic contact dermatitis include nickel, plants like poison ivy, and chemicals found in personal care products. It’s not just nature that triggers it, but also man-made substances.
In the case of irritant contact dermatitis, the key culprits are solvents, detergents, hair products, soaps, and various chemicals. Other triggers for contact dermatitis include hair dyes, certain antibiotics, preservatives, and chemicals. It’s indeed a tricky skin condition to navigate.
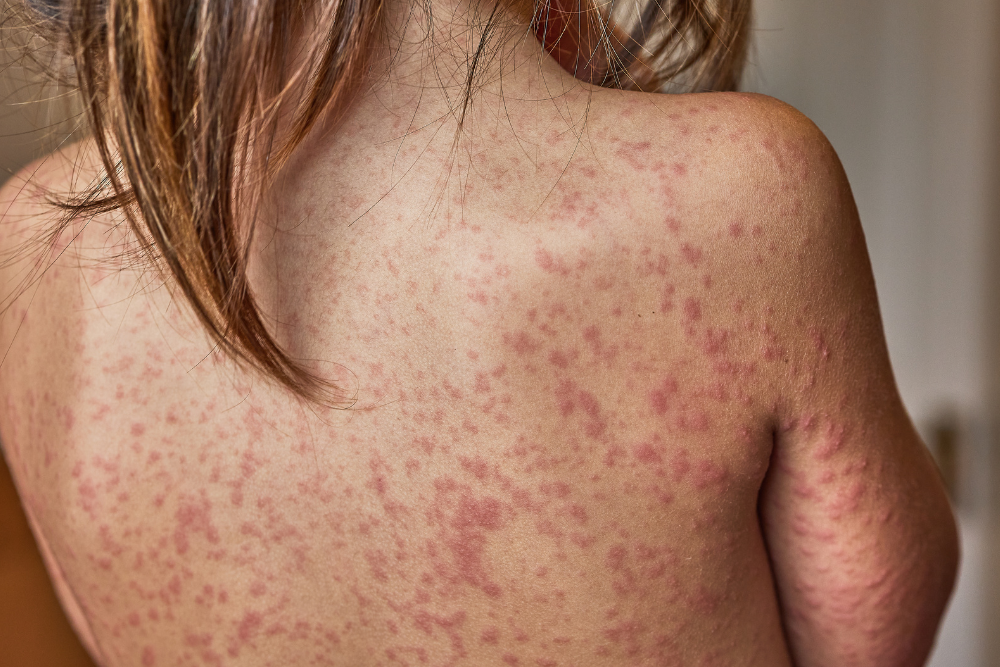
Symptoms
Contact Dermatitis commonly manifests as:
A red rash
Cracked skin
Blistering
Thickened patches
Dryness
Intense itchiness
However, symptoms can appear differently on various skin tones. Brown or black skin may display leathery patches darker than the surrounding skin, while white skin shows dry, cracked, and scaly patches.
Keep in mind that the rash associated with contact dermatitis can develop within just minutes to hours after contact with the irritant and may persist for 2 to 4 weeks. It’s a skin condition that demands immediate attention.
Treatments
When it comes to soothing the rash associated with contact dermatitis, steroid creams or ointments can be used. In severe cases, oral medications may be prescribed to reduce swelling, relieve itching, or address bacterial infections.
Effective self-care for Contact Dermatitis includes:
Keeping nails short to prevent scratching and breaking the skin
Using anti-itch creams
Taking oral antihistamines
Applying cool, wet compresses
Relief from contact dermatitis symptoms at home can be achieved by following these self-care measures.
Moisturisers play a key role in managing contact dermatitis, especially for those with sensitive skin, by restoring the skin’s barrier and keeping the skin supple.
Other Types of Eczema: Beyond Atopic and Contact Dermatitis
While atopic dermatitis and contact dermatitis are the most common types of eczema, other types are more prevalent in adults, such as discoid eczema. Seborrheic dermatitis usually presents with scaly patches, dandruff, and red skin, primarily affecting oily areas like the scalp, face, sides of the nose, eyebrows, ears, eyelids, and chest.
Dyshidrotic eczema is characterised by small, painful, fluid-filled blisters on the hands and feet, with causes potentially linked to stress, allergies, and exposure to certain metals. Varicose eczema typically affects the lower body and occurs due to poor circulation. These types serve as a reminder that dermatitis and eczema cover a wide range of skin conditions, each with unique causes, symptoms, and treatments.
Risk Factors and Triggers

While the types of dermatitis and eczema vary, the risk factors and triggers often overlap. A family history of eczema, allergies, hay fever, or asthma increases the risk of developing atopic dermatitis and other eczema types. Certain demographics, such as female gender, have higher incidences of atopic dermatitis.
Exposure to environmental irritants like smoke, air pollutants, harsh soaps, wool fabrics, skincare products, and low humidity can trigger eczema flare-ups. Additionally, common household items like cleansers, detergents, certain lotions, and solvents are known to worsen dermatitis and eczema conditions. Eczema symptoms can worsen upon exposure to allergens like dust mites, pollen, pet dander, and certain foods, which may also trigger related conditions such as hay fever.
Lastly, stress and lifestyle factors, including fatigue and seasonal changes, can influence the occurrence of eczema.
Prevention and Management Strategies
So, how do you handle these pesky skin conditions? Prevention and management strategies are key. Here are some tips to help:
Moisturise the skin at least twice a day to reduce dryness and maintain skin health, even when eczema is not active.
Use gentle washing techniques with mild unscented soaps.
Manage exposure to cold weather.
Regularly apply bath oils in cool baths to improve skin condition.
Identify and steer clear of personal eczema triggers, which can include:
Materials like wool
Chlorine
Heat and humidity
Harsh chemicals
Allergens that also trigger hay fever
Using protective measures such as gloves, avoiding harsh chemicals, and staying away from allergens can minimise the risk of eczema flare-ups. Stress and lifestyle factors, including fatigue and seasonal changes, can also influence the occurrence of eczema, and proactive management of these factors can aid in flare-up prevention.
Lastly, develop a personalised eczema action plan with a healthcare provider, which may include the strategic use of topical steroids, emollients, wet dressings, and allergy shots.
Diagnosing Dermatitis and Eczema
Self-care can often resolve minor cases of dermatitis, making it unnecessary to seek medical treatment. Taking simple steps such as avoiding triggers and using over-the-counter creams can help manage the condition. However, persistent or severe symptoms warrant a visit to your general practitioner (GP) or dermatologist for proper diagnosis and treatment. The diagnosis of atopic dermatitis and contact dermatitis typically involves a physical exam, discussing symptoms with a healthcare provider, and reviewing medical and family history.
Patch testing is a key test to assess for allergic contact dermatitis, whereby a panel of allergens is customised for each patient, and reactions are monitored over several days. Blood tests can reveal atypical immunoglobulin E levels for people with extrinsic atopic dermatitis, assisting in diagnosis. In some cases, skin biopsies may be conducted to differentiate dermatitis from other skin diseases, providing a clear diagnosis.
Diagnosing the exact cause of contact dermatitis can be challenging as symptoms can appear days after exposure to the allergen.
Comorbidities and Related Conditions
It’s important to note that dermatitis and eczema don’t exist in a vacuum. Asthma and eczema are both inflammatory conditions with a genetic predisposition, causing individuals to potentially suffer from both. The ‘atopic march’ describes the progression where children with eczema often develop hay fever and asthma as they grow older.
To manage eczema and asthma effectively, reducing exposure to shared allergens and following a medication plan is important. Atopic dermatitis can lead to complications such as bacterial and viral skin infections as well as eye conditions like conjunctivitis and blepharitis. It’s indeed a whole-body concern, not just a surface issue.
Summary
From the itchy red patches of atopic dermatitis to the allergic reactions of contact dermatitis, skin conditions are vast and complex. By understanding the differences, causes, symptoms, treatments, and risk factors, you can better manage these skin conditions and improve overall skin health. Remember, your skin is your body’s largest organ. It deserves as much care and attention as your heart, lungs, or brain.
Frequently Asked Questions
What is the difference between dermatitis and eczema?
Eczema is a type of dermatitis, which is a broader term encompassing more than just eczema rashes. Both lead to itchy, dry, and inflamed skin, but atopic dermatitis (commonly known as eczema) is a specific type of inherited, chronic inflammatory skin condition.
What are the 3 types of dermatitis?
The three types of dermatitis are allergic contact dermatitis, irritating contact dermatitis, and atopic dermatitis. These forms of dermatitis can cause symptoms such as itching, dryness, rash, blistering, and flaking skin.
Does dermatitis go away?
Dermatitis can often be managed with treatment and by avoiding irritants, but it can be a long-term condition, especially for adults. In some cases, it may go away on its own, but managing symptoms is key.
What are the common triggers of dermatitis and eczema?
Common triggers of dermatitis and eczema include environmental irritants such as smoke, air pollutants, harsh soaps, wool fabrics, skincare products, and low humidity. Additionally, symptoms can worsen with exposure to allergens like dust mites, pollen, pet dander, and certain foods.
How is Dermatitis diagnosed?
To diagnose dermatitis, a healthcare provider will conduct a physical exam, discuss symptoms with you, and review medical and family history. In some cases, patch testing, blood tests, or skin biopsies may be used to confirm the diagnosis.





