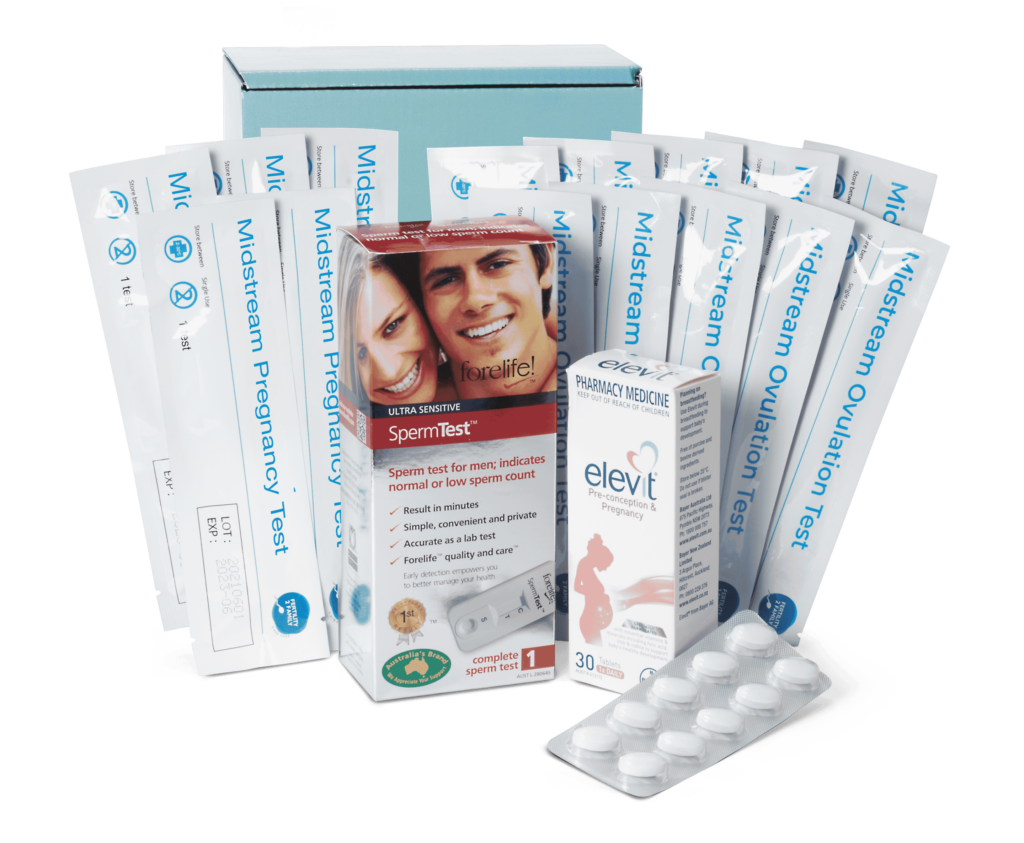
You’ve decided to have a baby – congratulations!
Pregnancy is a complex process that requires synchronicity of many lifestyle factors and biological processes. Wherever you are in your journey, the following information will help you to organise your life and optimise your health for improved chances of conception.
understanding fertility and ovulation
Fertility 101
Fertility refers to the ability to have a baby and it can be impacted by many different factors. Being informed about ovulation and the ‘fertile window’ can dramatically improve your chances of getting pregnant.
What is ovulation?
Ovulation is a key stage of the menstrual cycle. During ovulation a mature egg is released from one of the ovaries in preparation to be fertilised by a sperm. Understanding ovulation will help you to fall pregnant faster by detecting your most fertile time, commonly called your fertile window.
The fertile window
Conception is only possible for about five days before ovulation through to the day of ovulation. These six days are considered the fertile window of your menstrual cycle, and they reflect the five-day lifespan of sperm and the 24-hour lifespan of an egg. Timing sex to align with your fertile window is a crucial step of the pre-conception stage of pregnancy.
How to know when you’re ovulating?
Now that you know the ideal time for sex is during your fertile window, it’s important to learn how to recognise when you’re ovulating. Start by working out the length of your cycle, and then identifying the physical changes your body experiences before and during ovulation.
Working out your fertile window
To work out the length of your cycle, count the days from day one of your period to the first day of your next period. The average cycle is 28 days, with some women experiencing longer or shorter variations. If you have a period every 28 days, you will ovulate around day 14, so your fertile window will be between days 11 to 14. If you have a shorter cycle of 24 days, you will ovulate around day 10, and your fertile window will be between days 7 and 10.
Physical changes and signs of ovulation
Ovulation pain
Mild pain in the abdominal area can occur a day before, during and after ovulation. Pain should only be mild, not severe.
Since abdominal pain can be a sign of ovarian cyst rupture, pelvic adhesions, endometriosis, and other health conditions, it isn’t considered a reliable method to track ovulation.
A drop in basal body temperature (BBT)
Basal body temperature drops prior to ovulation before quickly increasing after ovulation. Monitoring your menstrual cycle daily is essential to tracking your BBT. That means you need to check your body temperature every morning at the same time.
Since BBT can be influenced by many other factors (stress, fevers, medications) it isn’t a reliable method of tracking ovulation.
A surge in luteinizing hormone (LH)
As you move closer towards ovulation, your level of luteinizing hormone increases to assist with the release of the egg from the ovary. This is called the LH surge, and ovulation will occur 24-36 hours after it happens.
Ovulation predictor kits are reliable urine-based tests that can help detect upcoming ovulation by measuring the levels of luteinizing hormones in your urine.
Changes in cervical mucus
One of the easiest signs of ovulation to recognise is a change in your cervical mucus. During ovulation, vaginal discharge is likely to be stretchy, slippery, clear, and similar in texture to raw egg whites. You may spot a change in vaginal mucus when urinating, or in your underwear.
Changes in cervix position
As ovulation nears, the cervix tends to move higher into the body as it becomes softer and moist. Changes in cervix positioning can only be measured with fingers, making this method of detecting ovulation unreliable.
Changes in saliva
As ovulation approaches, oestrogen levels increase and coincide with an increase in sodium levels. These saliva changes are known as ferning or crystallisation, because under a microscope the saliva will appear as a fern leaf or frosty snowflake.
An increased libido
As the female body approaches ovulation, it can experience an increase in sex drive. Sometimes a female body just intuitively knows what it needs to do to procreate.
Age matters
There’s no sugar-coating the fact that age is the most important factor when it comes to fertility. You’re only granted a certain number of eggs at birth. The more healthy eggs you have, the higher the likelihood of ovulation occurring and turning into a healthy pregnancy. As you age, the quality and quantity of your eggs starts to decline in a non-reversible fashion. The chances of conception decrease with age, with women younger than 35 and men younger than 40 having a better chance of pregnancy than people who are older.
preconception checklist
for women
Stop using contraception
If you haven’t made the transition towards contraception-free intercourse, now is the time. Speak with your doctor if you’re concerned about any side effects and ways to manage them.
Maintain a healthy body weight
Being in the healthy weight range increases your chance of conceiving and having a healthy baby. If you’re overweight, losing even a small amount of weight (3-5kg) can improve fertility and reduce the risk of pregnancy complications.
As a general guide, a healthy weight for conception is:
- A body mass index (BMI) between 18.5 and 24.9, or
- A body fat percentage between 22-25%
Being outside these ranges doesn’t mean you can’t conceive; it just makes it slightly harder for you to conceive.
Get physically active
Being in the healthy weight range increases your chance of conceiving and having a healthy baby. If you’re overweight, losing even a small amount of weight (3-5kg) can improve fertility and reduce the risk of pregnancy complications.
Studies have shown that moderate exercise is beneficial for general health and improving fertility. Aim to achieve 30 minutes of moderate physical activity (brisk walking, jogging, swimming) per day.
Eat a fertility-enhancing diet
A well-balanced diet can help nourish and prepare the body for conception. If seeking inspiration, a Mediterranean style diet is a great place to start, with studies showing that a Mediterranean style diet may improve fertility. That looks like:
- Plenty of fruit and high-iron vegetables
- More white meats, like chicken and fish, and less red meat
- Legumes, like beans, tofu, and nuts
- Replace oils with vegetable oils
- Avoid highly processed foods, trans fats, and sugars
Cut back on the caffeine
Caffeine is okay in small amounts. Some research suggests that women who consume large amounts of caffeine may take longer to conceive. Aim to consume 200 mg or less of caffeine per day.
To ensure you manage your preconception caffeine hit:
- 1 shot of espresso = 100 mg
- 1 cup of black tea = 48 mg
- 1 cup of green tea = 29 mg
- Matcha = 70 mg
- Standard can of cola = 49 mg
Track your ovulation
Ovulation is the best time to have sex to get pregnant. Learning exactly when you’re ovulating can be tricky. Period and cycle tracking apps can help remove ovulation date guesswork by monitoring how many days your cycle lasts, individual signs of ovulation, cycle symptoms, and personalised insights.
Start with:
- Flo Period and Cycle Tracker
- MyFlo Tracker
- Clue Period Tracker
Take a prenatal supplement
To optimise your chances of falling pregnant, nutritional experts recommend taking a prenatal supplement 3 months before you start trying to conceive. The initial weeks of a baby’s life are critical, with the development of some of the most important organs taking place. Consuming a daily prenatal supplement with 400 mg of folic acid and 150 mg of iodine will help to reduce the risk of some serious birth defects and provide adequate nourishment for the baby during the earliest days of conception (before you’re even aware you’re pregnant).
Book a dental check-up
Gum disease can impact the health of you and your baby during pregnancy. Try to schedule a dental check-up, clean, and any treatments before you start trying to conceive
Manage existing health conditions
Some medical conditions, such as PCOS, endometriosis, diabetes, and sexually transmitted infections (STIs) can affect fertility. Seek advice from your doctor regarding the management of any existing medical conditions and medications you’re taking.
Book a preconception check-in with your doctor
Seeing your doctor for a check-up can help ensure you’re as healthy as possible before trying to conceive. Your doctor can also confirm your vaccination status, so you have proper immunity against infections that could potentially harm your baby.
preconception checklist
for men
Take a prenatal supplement
It takes two humans to create a little bundle of joy, and a male prenatal supplement can help to improve sperm health and mobility. Thus, improving your chances of getting pregnant sooner.
Consider male fertility testing
The function of a sperm test is to analyse a man’s semen to identify sperm quantity, sperm mobility, sperm quality, and the volume and consistency of ejaculatory fluid. You wouldn’t jump in a car with a flat tyre and expect to reach your destination. The same concept applies with male fertility, and a sperm test will help to improve any issues that appear during testing.
Things to Avoid When Trying to Conceive
Some skincare products
Some prescription skincare products, like retinoids, retinol, and vitamin A, can be dangerous for babies. Check in with your doctor or skin care specialist if you’re unsure about the effect of your skin care regime on your baby.
Need help with skincare? Chat with a doctor for prescription skincare based on your skin type and pregnancy plans.
Alcohol
According to the Royal Australian and New Zealand College of Obstetricians and Gynaecologists (RANZCOG), alcohol can be detrimental towards a baby’s growth and development. To be safe, stop drinking alcohol when you first start trying to conceive.
Cigarettes
Studies have shown that women who smoke are more than 50% less likely to conceive naturally when compared to non-smokers.
Smoking, vaping, and other nicotine products can also increase the risk of miscarriage, preterm birth, low baby birth weight, birth defects, sudden infant death syndrome (SIDS), asthma, and other respiratory conditions.
For advice and assistance to quit smoking, visit Quitline.
Recreational drugs
Recreational drugs, like marijuana, cocaine, speed, heroin, ice, LSD, and methadone can cause serious harm to unborn babies. They can also increase the risk of miscarriage, preterm birth, and stillbirth.
For support on giving up recreational drugs, visit the Alcohol and Drug Foundation.
Plastics
Bisphenol-A, more commonly known as BPA, is a chemical used to make plastics hard and break-proof. BPA can disrupt the endocrine system, an important part of the body that directly impacts fertility. You’ll find BPA-free plastics, glass, and stainless steel to be safer options.

Elevit Pre-conception & Pregnancy Multivitamin
A multivitamin and mineral supplement specially formulated to support increased nutritional requirements of women during pregnancy.
What are the key benefits of Elevit Preconception & Pregnancy Multivitamin?
During the first eight weeks of pregnancy, the critical development of vital organs takes place. For your body to support these developments, it requires higher levels of certain nutrients.
What is the dosage?
Elevit Preconception & Pregnancy Multivitamin is a small once daily tablet that can be taken at any time of the day. For best results, start taking Elevit from at least one month prior to conception and throughout pregnancy.
More information and ingredients of Elevit Preconception & Pregnancy Multivitamin

F2F Midstream Ovulation Test
The Fertility2Family Midstream Ovulation Test is a fast and easy-to-use method of predicting the time of ovulation and your most fertile window! During this window, pregnancy is most likely to occur. The Fertility2Family Midstream Ovulation Test detects the Luteinizing Hormone (LH) surge which occurs 12 to 48 hours prior to ovulation, signalling the best time to have intercourse to achieve pregnancy.
When to begin testing?
First, you must determine the length of your menstrual cycle. This is the number of days from the first day of your menstrual bleeding to the day before your next bleeding begins again. Please refer to the chart to determine when you should start testing.
If your cycle is shorter than 21 days or longer than 38 days, consult your doctor. If you do not know your cycle length, you may begin testing 11 days after your first period, as the average cycle length is 28 days. Perform 1 test each day over a 5- day period or until the LH surge has been detected.
Urine collection
- Do not use first morning urine samples as LH is normally made in your body early in the morning.
- The best time to collect your urine is between 10am-8pm.
- Collect urine at approximately the same time each day.
- Reduce liquid intake approximately 2 hours before collecting your urine as a diluted sample can prevent the test from detecting your LH surge.
Test procedure
- Remove the test stick from the foil wrapper.
- Remove the cap to expose the absorbent tip, avoiding contact with the absorbent end.
- Hold the stick by the thumb grip with the exposed absorbent tip pointing downward. Urinate onto the absorbent tip only until it is thoroughly wet.
- Recap the device and lay the test stick down on a flat surface with the window facing up.
Interpretation of results
While you are waiting for your results, you may notice a coloured solution moving across the windows. This is normal. Positive results may be observed in as short as 40 seconds. However, to confirm negative results, the complete reaction time of 10 minutes is required. To determine your results, compare the colour intensity of the test line to the control line as follows:
Negative (No LH surge):
Only one colour band appears on the control region, or the test line is lighter than the control line.
Positive (LH Surge):
If two colour lines are visible and the test line is equal to or darker than the control line, you will likely ovulate in the next 12-48 hours.
Invalid:
If a control line does not appear, the test is invalid. Insufficient specimen volume or incorrect test performance is the most likely reason. Repeat test with a new test kit.
More information and FAQs on Fertility 2 Family Midstream Ovulation Tests.

F2F Midstream Pregnancy Test
Fertility2Family Midstream Pregnancy Tests are a fast, reliable, and easy-to-use method of detecting pregnancy. The Fertility2Family Midstream Pregnancy Test detects the hCG (human Chorionic Gonadotropin) hormone. A hormone which is produced after the fertilised egg adheres to the wall of the uterus.
Start testing from 7 days past ovulation.
How to perform a midstream pregnancy test?
- Remove the test stick from the foil wrapper.
- Remove the cap to expose the absorbent tip, avoiding contact with the absorbent end.
- Hold the stick by the thumb grip with the exposed absorbent tip pointing downward. Urinate onto the absorbent tip only until it is thoroughly wet.
- Recap the device and lay the test stick down on a flat surface with the window facing up.
- Results may be observed after 1 minute. Do not interpret test results after 5 minutes.
- Discard the test device after single use.
Interpretation of results
Negative: If only one coloured line appears in the control area, the test is negative, and you can assume that you are not pregnant.
Positive: If two coloured lines appear both in the control area and test area, the test is positive, and you can assume you are pregnant.
Invalid: If there is no distinct pink-purple coloured band visible both in the test area and control area, the test is invalid. It is recommended that you should retest, using a new test stick. If the problem persists, contact Fertility2Family.
More information and FAQs on Fertility 2 Family Midstream Pregnancy Tests.
Preconception Pack
Kick-start your fertility journey with our Preconception Pack.
Includes the essentials to support fertility and conception for women.
– Only $80/month
– Free, discreet delivery
– Cancel anytime